
Aged care homes ask for children to send letters to residents
April 13, 2020
Military nurse & mother-of-two chosen to address the nation in Anzac Day service
April 22, 2020Insights from an Australian humanitarian nurse on the pandemic frontline
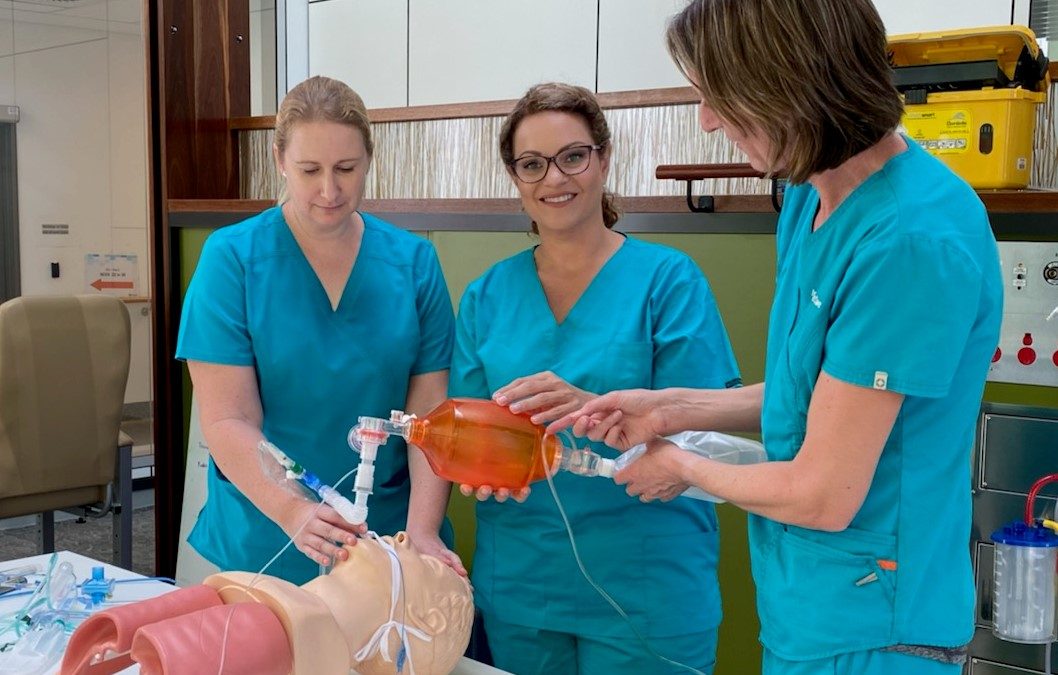
Insights from an Australian humanitarian nurse on the pandemic frontline
Helen Zahos is an Australian emergency nurse and paramedic who is currently working at the Gold Coast University Hospital intensive care unit with COVID-19 patients. She has extensive experience as a humanitarian volunteer overseas responding to disasters and emergencies, and with refugees. Most recently she joined the Nurses in Action Program in rural Kenya.
She was interviewed after her return to Australia.
Please tell us some of the key things you have taken away from your recent volunteer stint in Kenya with the Nurses in Action Program?
That the disparities in health care between developing countries and developed countries are ever present and that volunteer programs have to maintain a focus on sustainability and involve community members so they are empowered. That education and sharing your knowledge is an integral part of humanitarian nursing, as it is through sharing your skills and knowledge that you empower local Kenyan nurses. In turn they educate the locals in the community and encourage them to access the care they need.
How is it similar or different from your earlier experiences working with refugees overseas?
The experience was very different. The refugee crisis was a slow-moving disaster. It overwhelmed specific countries that could not cope with the influx of people and it exceeded the capabilities of existing resources and infrastructure. The refugees were on the move and fleeing conflict, they were not living in homes but in refugee camps. Health care issues included chronic conditions but also physical and emotional trauma.
While Kenya is one of East Africa’s most advanced and richest countries, poverty is common. Deeply seeded systemic issues in health care mean that many people lack access to medical facilities or they cannot afford to seek treatment. There are endemic diseases such as malaria and HIV affecting many people. With limited funding or resources, it is often up to civil society to fill in the gaps and assist.
You have returned to critical care nursing in an Intensive Care Unit in Australia at an incredibly difficult time. Have you experienced the impact of COVID-19 as yet?
My hospital has COVID-19 patients and the Intensive Care Unit does as well. It can be daunting as you approach the area where you get changed and approach the area that is separated from the COVID-19 patients because of the seriousness of this virus and how easily it spreads. It is hot under the Personal Protective Equipment (PPE), the masks are tight and claustrophobic and it is hard to talk to patients.
What are the most pressing priorities for the Australian hospital system? For nurses and other health workers?
To source more staff; have them trained and ready; source equipment and increase supplies. To put into practice the guidelines for pandemics. We have been preparing for the worst.
Integration and communication are vital: training and preparing all staff involved in the hospital system, transparency and sharing of information to assist other countries and standardising triage and treatment systems to cope with an influx of patients. Conducting mass screening and testing in the community by running fever clinics have been essential for early detection.
What about the challenges facing indigenous communities at this time?
The possibility of a pandemic spreading to and affecting our remote indigenous populations is really concerning and very possible. Our indigenous people have higher co-morbidities and lower life expectancy than non-indigenous Australians. We could see the demise of entire indigenous communities if COVID-19 spreads to these remote areas, where large families live in close proximity, there are mass gatherings for cultural practices and they tend to be nomadic.
The Northern Territory has led the way by closing its borders and access to remote areas, important steps in stopping the spread of the virus. Remote area health centres need to be vigilant and detect any cases early, to educate indigenous people about the virus and to conduct health promotion on hand washing and social distancing.
Any advice for the rest of us? or suggestions for how we can help?
Accept that you have no control over this situation. What you do have control over is how you respond. Stay at home, wash your hands and practice social distancing. If you are self-isolating use this time in a positive way. Limit yourself to the news or to the daily updates as it can be distressing. Take time for self-care which is difficult when you are exhausted mentally. If you are isolated from family there are many social media groups that have been created; if you are unable to get out to access groceries or pick up a script there are people in the local community volunteering to help. Write a diary of how you are feeling, the events unfolding and take photos of what is happening. This is vital for debriefing and looking back at this time, years down the track.
How do see your role as a nurse during the International Year of the Nurse and the Midwife, during the pandemic?
The International Year of the Nurse means a lot to me; I was there when they announced it at the World Health Assembly in Geneva. I remember feeling really proud to be a nurse. Then came the announcement that I was to be an ambassador for Nurses in Action for World Youth International and I was excited to partner up with them. I will cherish the trip to Kenya forever.
There are countries, where people cannot buy soap and do not have access to running water, that will suffer the most. It is these vulnerable populations that will need nurses to volunteer again one day to help in their recovery.
I never imagined that the year of the nurse would take on such a different meaning.
This article was originally published on Global Voices on 8/4/2020 by Kevin Rennie.










